Archive \ Volume.11 2020 Issue 4
IL 1α +4845, IL 1β +3954, and TNF α-308 Gene Polymorphisms in Patients with Aggressive Periodontitis
Fatima Ali Ahmed Alhag 1, Wafaa Mohammed Eltazi 2, Ibrahim Ahmed Ghandour 2, Sara Abdelghani 3, Yousif Mohammed, Elmosaad 4, Hisham Ali Waggiallah 5, Lienda Bashier Eltayeb 5*
1 Department of Periodontology, Faculty of Dentistry, Al Neelain University, Sudan. 2 Department of Periodontology, Faculty of Dentistry, University of Khartoum, Sudan. 3Department of parasitology. Faculty of Medical Laboratory Sciences, Al- Neelain University-Sudan.4 Department of Public Health, College of Applied Medical Sciences, King Faisal University, KSA. 5 Department of Medical Laboratory Sciences, College of Applied medical sciences, Prince Sattam Bin Abdul-Aziz University, KSA.
Abstract
There is conclusive proof that genetic, bacteriologic, immunologic, and ethnic factors influence the onset of Periodontitis. The study aimed to investigate the role of single nucleotide gene polymorphisms of IL 1α +4845, IL 1β +3954, and TNF α-308 gene polymorphisms in Sudanese patients with aggressive periodontitis. Among 4.688 patients examined only 95 patients were diagnosed as aggressive periodontitis subjects, and 95 apparently healthy as control. A volume of 5 ml of venous blood was obtained, then preserved in EDTA vacutainers, and was used for genotyping assays using polymerase chain reaction and restriction fragment length polymorphism technique. The overall prevalence of aggressive periodontitis was 2%. Females had a higher aggressive periodontitis prevalence (1.6%), it is more prevalent among Sudanese from western states (38.9%), also (68.1%) of patients were of African origin. There was a significant correlation in all clinical parameters regarding GI, CAL, PD, and RI in AgP patients and control. The homozygous IL-1α (+ 4845) allele 1 was revealed in 53 (55.8%) of the control group and 16 (16.8%) of the age group. Homozygous allele1 of IL-1β was closely similar between patients and control (47(49.5%), vs 46(48.4%), respectively). Regarding allele 1 and 2 frequency (no statistically significant difference for IL-1β), homozygous allele 2 of TNF-α was more prevalent in the AgP group. A significant correlation was revealed between pocket depth and IL1-α, IL, and TNFα. This study provides a significant clue that the IL-1α and IL-1β gene polymorphisms are correlating with AgP in the Sudanese population, the genotype of IL-1α remains a considerable risk factor for AgP. The study revealed a high prevalence rate of aggressive periodontitis (2%), and it is a significantly age-, gender-, and ethnic-associated disease.
Keywords: Aggressive Periodontitis, ethnic, demographic, Africans, Afro-Arab
INTRODUCTION
Pro-inflammatory cytokine interleukin-1 (IL-1) cluster and TNF gene polymorphisms are the primary regulators of the immune response to microbial infection, which play a crucial role in the extracellular matrix catabolism and bone resorption, have been associated with an increased risk of developing serious adult periodontitis [1, 2]. Periodontitis is a complex, multi-factorial infectious disease where rapid destruction of the periodontal ligament and alveolar bone that generally occurs in a younger age group [3, 4]. It is categorized into two major forms of chronic periodontitis (CP) and aggressive periodontitis (AgP) [5]. The incidence of aggressive periodontitis has been documented to be less prevalent than that of chronic periodontitis, early tooth loss in affected individuals may occur if not identified early and treated accordingly. AgP is encountered to have an ethnic and sexual tendency, with blacks and female teenagers at greater risk of being infected relative to whites and males [6]. In addition to the existence of multiple risk factors related to the development of periodontitis, immunological, genetics, as well as environmental factors, influence the early onset, seriousness, and progression of periodontitis [7]. Destruction of periodontal ligament emerges via a complicated interaction of bacterial biofilm (Aggregatibacter actinomycetemcomitans and some population of Prophyromonas gingivalis) and host response [8], which is incompatible with the magnitude of periodontal tissue destruction, as well as phagocyte disturbances and ultra-responsive macrophage phenotype, particularly increased interleukin-1β levels. These bacteria produce leukotoxin, which destroys neutrophils and macrophages that trigger and secrete proteases and interleukin-1β (IL-1β) respectively, then reduce the response of the host and potentially lead to periodontal breakdown [9].
In recent years, studies have shown that periodontitis is associated with significantly higher levels of a variety of inflammatory biological markers and they especially focus on genes of immunoregulatory molecules, such as cytokines, chemokines, membrane surface receptors, and antigen recognition proteins. Proinflammatory cytokines IL-1 and TNF-α are considered significant mediators of the progression of periodontal inflammation, differentiation, and activation of B lymphocytes, inflammatory infiltrate, and stimulation of osteoclasts [10, 11]. Polymorphisms in these molecules have been suggested as factors that influence the risk of developing the disease.
A significant correlation between periodontitis and composite genotype, namely, allele 2 of a single nucleotide polymorphism (SNP) of IL-1A+4845 and IL-1B+3954 located on chromosome 2q13. Then, various studies have been proceeded evaluating the role of IL-1 gene polymorphism as a possible factor in periodontitis in various populations and ethnic groups [12, 13]. Gene polymorphisms expressing interleukin (IL)-1 are the most genes associated with polymorphisms in periodontitis research [14]. IL-1α and IL-1β, located in the long arm (q arm) of chromosome 2 are the most critical identified ones among at least ten molecules that are associated with the pathogenesis of periodontitis. IL-1α binds to the cell surface, and IL-1β is released into the environment [15]. They involve a variety of mechanisms necessary to initiate and maintain an inflammatory response, this stimulates the development of adhesion molecules, promotes the movement of leukocytes, stimulates the synthesis of other inflammatory mediators and metalloproteinases, activates T and B lymphocytes, induces osteoblasts leading to bone resorption, and activates apoptosis of cells, thereby reducing the regenerative ability of tissues [16].
Tumor necrosis factor-α (TNF-α) is one of the most potent pro-inflammatory cytokines, which plays a major role in tissue injury and induces bone resorption in the immune system, located at the short (p) arm of chromosome 6 at position 21.3. It triggers several immune and inflammatory mechanisms, as well as plays roles in necrosis and apoptosis. Bacterial pathogens of dental plaque stimulate the secretion of TNF-α, which causes osteoclast differentiation and results in bone resorption. Genetic analysis has revealed a large number of single nucleotide polymorphic (SNP) sites within the TNF-α locus that are related to periodontitis [17, 18]. As there are no consistent data on the prevalence of aggressive periodontitis in Sudan, as well as genetic analysis among AgP, the present study aimed to investigate the distribution of IL-1 (IL 1α+ 4845, and IL1β+3954), and TNF gene polymorphism in aggressive periodontitis in the Sudanese population.
MATERIAL AND METHODS
Study population:
A case-control study was conducted among Sudanese patients with aggressive periodontitis attending Khartoum Teaching Dental Hospital, Sudan. Ethnic disparities existed because Khartoum Teaching Dental Hospital is the main hospital for all Sudan states. Ethical approval was taken from the institutional review board, Faculty of Dentistry Al-Neelain University. Participants enrolled in the study after signing informed consent and being notified about their illness.
Criteria of selecting patients with aggressive periodontitis were as follows: Age range from 10-29 years, scanty plaque deposit, pocket depth ˃3mm attachment loss ≥3mm around incisors and first molars, tooth mobility or pathological migration. Any patient with the following systemic diseases was excluded, Dawn’s syndrome, leukemia, cyclic neutropenia, and diabetes mellitus. Patients used antibiotic for last 3 months were also excluded. Panoramic and per apical radiographs were used to confirm the diagnosis wherever needed. All demographic data such as gender, age, ethnic, and regional distribution of the patients were documented. In addition, the type of whether the case was a generalized or a localized one was also determined. A total of 4688 patients were screened for AGP, among them, 95 were diagnosed as AGP subjects and have been recruited in the study along with 95 health subjects as control.
Samples collection and DNA extraction protocol:
A total of 95 blood samples were collected from the participants. For genomic extraction of DNA, a 5-ml peripheral blood sample was obtained from each subject in the EDTA anticoagulant containers. DNA was extracted from the whole blood using the phenol/chloroform extraction method and stored at +4°C until genotyping. DNA extracts were analyzed by conventional polymerase chain reaction (PCR) using suitable primers for IL-1α+ 4845, IL-1β+3954, and TNFα-308. All output results were viewed by electrophoresis using 3% agarose gel, staining with ethidium bromide, and photographing with an ultraviolet radiation transilluminator (Table 1, summarized PCR condition).
|
Table 1: Polymerase Chain Reaction condition. |
||||
|
Cytokines |
Primers |
PCR Condition |
products |
Enzymes |
|
IL 1α (+ 4845) |
F 5’ ATG GTT TTA GAA ATC ATC AAGCCT AGG GCA 3’ R 5’ AAT GAA AGG AGG GGATGA CAG AAA TGT 3’ |
45 cycles, cycling at 94°C for 1 min, 94°C for 1 min, 56°C for 1 min, 72°C for 2 min, and 72°C for 5 min. |
124 bp+29bp1/1 153bp 2/2 153 bp, 124 bp, and 29 bp/1,2 |
Fnu4HI |
|
IL1β (+3954) |
F 5’ TC AGG TGT CCT CGA AGA AAT CAA A R 3’ and 5’ GCT TTT TTG CTG TGA GTC CCG 3’. |
35 cycles cycling at 95°C for 2 min, 94°C for 1 min, 53°C for 1 min, and 72°C for 1 min |
97 bp+85 bp 1/1 182 bp 2/2 182bp+97bp+85 bp 1,2 |
Taq I |
|
TNFα (-308) |
F 5’ TGG CAT TGA TCT GGT TCA TC R 3’ and 5’ TTC TCC CTG CTC CGA TTC CG 3’. |
35 cycles, cycling at 94°C for 3 min, 60°C for 1 min, 72°C for 1 min, and 60°C for 1 min. |
87 bp and 20 bp 107 bp 107 bp, 87 bp, and 20 |
NcoI |
Statistical Analysis:
Statistical analysis of the data was conducted with the SPSS software version 20.0. In addition to descriptive statistics (e.g., frequency and percentage), chi-square test, were used. The threshold for statistical significance was p < 0.05.
RESULTS:
Baseline characteristics:
A total of 4688 patients were screened (1563 males and 3125 females). only 95 were diagnosed as aggressive periodontitis, 18 (18.9%) of them were males with a prevalence rate of 0.4%, and 77 (81.1%) were females with a prevalence rate of 1.6%. The overall prevalence of aggressive periodontitis among all patients examined was 2% (Table 2).
(Table 3) shows the baseline distribution of demographic features among aggressive periodontitis and control groups. The age groups ranged from 10 to 29 years old, female participants were significantly higher among patients and control groups (77 (81.1%) and 54 (56.8%), respectively). African tribes had a significantly higher prevalence of aggressive periodontitis compared to Afro-Arab tribes (68.4% vs 31.6%). Regarding the distribution of participants according to their region of origin, subjects from the western states constituted 38(39.0%), followed by northern, central, and eastern states (33 (34.7%), 21(22.1%), and 3(4.2%) of those with aggressive periodontitis, respectively). About 52 (54.7%) patients brush their teeth once a day, there was a significant correlation (P-value 0.000) regarding plague and mobility among the patient and control groups.
There are significant correlations in all clinical parameters regarding GI, CAL, PD, and RI in AgP patients and control. The mean pocket depth index was 7.53±1.84, and 2.53±2.53 for aggressive periodontitis cases and control, respectively. The CAL estimated as the distance from the cementoenamel junction to the sulcus base was 2.04±2.50 mm for AgP and 6.44±0.57 mm for the control group. All data are summarized in (Table 4).
Distribution of genotypes and allele frequencies
The homozygous IL-1α (+4845) allele 1 was revealed in 53 (55.8%) of the control group and 16 (16.8%) of the AgP group, homozygous allele 2 and heterozygous allele (1,2) was predominant in AgP group 45 (47.4%), and 34 (35.8%), consequently. The differences between the two groups were significant (T. value =6.39, 95% Confidence Interval (0.44 -0.84). Allele 1 was more prevalent in both patients and control groups (65.3%, vs 52.6%), respectively. (Table 5).
Regarding IL-1β (+3954), the results of homozygous allele 1 were closely similar between patients and control groups (47 (49.5%), vs 46(48.4%), respectively). With regard allele 1 and 2 frequency, there is no statistically significant difference for genotype distribution (Confidence Interval -0.44-0.02) (P value=0.897). Data are displayed in Table 6.
As shown in Table 7, considering TNF, homozygous allele 1 and heterozygous allele 1,2 were much higher in the control group than the AgP group. In contrast, homozygous allele 2 was more prevalent in the AgP group, the frequency of allele 2 carriers was significantly more predominant (65.3%) among AgP, while allele 1 frequency was more predominant (89.5%) among the control group; P-value= 0.01). figure 1and 2 displayed IL-1α+4845, IL-1β+3954, and TNFα -308 PCR containing Single Nucleotide Polymorphisms and their corresponding restriction endonuclease digestion fragments after agarose gel electrophoresis.
Table 8 describes the genotype distribution of IL-1α (+4845), IL-1β (+3954), and TNF-α (-308) in AgP patients and healthy controls according to the gender. A significant correlation of IL-1α (+4845) genotype 1,1 carriers among males and females with AgP ((T. value=2.742, 95% CI=0.16-1.04), and (T. value= 5.425 95% CI (0.40-0.87) was revealed respectively), hence, the percentage of homozygous allele 1 of IL-1α (+4845) and IL-1β (+3954) were (44.5% vs 55.6%), respectively, and was more prevalent among males with AgP. Whereas, there was no significant correlation between TNF α (-308) genotypes distribution and gender. A significant correlation was revealed between pocket depth and IL1 α, IL,
and TNF-α Pearson correlation coefficient (-.036, .012, and -.006, respectively), nevertheless there was an association between the presence of CAL and IL1 α, and IL-1β only (Table 9).
|
Table 2: The Prevalence of Aggressive Periodontitis: |
|||
|
Gender |
Number screened (%) |
Number (%)-AgP |
Prevalence (%) |
|
Male |
1563 (33.3) |
18 (18.9) |
0.4% |
|
Female |
3125 (66.7) |
77 (81.1) |
1.6% |
|
Total |
4688 (100)% |
95 (100) |
2% |
|
Table 3: Baseline data between Patients AGP and control |
|||
|
Parameters |
Case ( N=95) |
Control (N=95) |
P. value |
|
Gender: (No. / %) |
|||
|
18 (18.9%) |
41 (43.2%) |
0.000 |
|
77 (81.1%) |
54 (56.8%) |
|
|
Age group (No. / %) |
|||
|
47 (49.5%) |
67 (70.5%) |
0.002 |
|
48 (50.5%) |
28 (29.5%) |
|
|
Ethnic group (No. / %) |
|||
|
65 (68.4%) |
29 (30.5%) |
0.000 |
|
30 (31.6%) |
66 (69.5%) |
|
|
Resident (No./ %) |
|||
|
|
15 (15.8%) |
0.067 |
|
|
31 (32.6%) |
|
|
|
30 (31.6%) |
|
|
3 (04.2) |
19 (20%) |
|
|
Hygiene (No. / %) |
|||
|
52 (54.7%) |
46 (48.4%) |
0.234 |
|
43 (45.3%) |
49 (51.6%) |
|
|
Plague (No. / %) |
|||
|
1 (1 %) |
32 (33.7%) |
0.000 |
|
56 (59%) |
48 (50.5%) |
|
|
38 (40%) |
11 (11.6%) |
|
|
0 |
4 (4.2%) |
|
|
Mobility (No. / %) |
|||
|
8 (8.4%) |
95 (100%) |
0.000 |
|
13 (13.7%) |
0 |
|
|
21 (22.1%) |
0 |
|
|
53 (55.8%) |
0 |
|
|
Table 4: Clinical Parameters among Study Groups |
||||
|
Parameters |
Case (mean ±SD) |
Control (mean ±SD) |
T. value |
95% Confidence Interval |
|
PD |
7.53±1.84 |
2.53±2.53 |
15.6 |
(4.4-5.6) ** |
|
GI |
1.16±0.55 |
0.78±0.62 |
4.4 |
(0.2-0.5) ** |
|
CAL |
8.89±1.85 |
2.04±2.50 |
21.5 |
(6.2-7.5) ** |
|
RI |
2.13±0.82 |
0.55±0.83 |
13.3 |
(1.3-1.8) ** |
**Statistically significant at p<0.001. Healthy controls; AgP: generalized aggressive periodontitis; PD: pocket depth; GI: gingival index; CAL: clinical attachment level; and RI Recession index
|
Table 5: Distribution of the IL-1α (+ 4845) genotypes and allele frequencies for study groups. |
||
|
Genotypes |
Case |
Control |
|
1,1 |
16 (16.8%) |
53 (55.8%) |
|
1,2 |
34 (35.8%) |
10(10.5%) |
|
2,2 |
45 (47.4%) |
32(33.7%) |
|
T. value (95% Confidence Interval) |
6.39 (0.44 -0.84)** |
|
|
Alleles Frequencies |
|
|
|
Allele 1 |
50 (52.6%) |
62 (65.3%) |
|
Allele 2 |
45 (47.4%) |
33 (34.7%) |
|
Total |
|
|
|
P. value |
0.236 |
|
|
Table 6: Distribution of the IL 1 β (+3954) genotypes and allele frequencies among the study groups. |
||
|
Genotypes |
Case |
Control |
|
1,1 |
47 (49.5%) |
46(48.4%) |
|
1,2 |
13 (13.7%) |
32 (33.7%) |
|
2,2 |
35 (36.8%) |
17(17.9%) |
|
t. value (95% Confidence Interval |
-1.79 (-0.44-0.02) |
|
|
Alleles Frequencies |
|
|
|
Allele 1 |
59 (62.1%) |
78 (82.1%) |
|
Allele 2 |
31 (32.5%) |
17 (17.9%) |
|
P. value |
0.897 |
|
|
Table 7: Distribution of TNF-α (-308) genotypes and allele frequencies among the study groups. |
||
|
Genotypes |
Case |
Control |
|
1,1 |
24 (25.2%) |
45(47.4%) |
|
1,2 |
9 (9.5%) |
40(42.1%) |
|
2,2 |
62 (65.3%) |
10(10.5%) |
|
T. value (95% Confidence Interval) |
-0.93(-0.34-0.12) |
|
|
Alleles Frequencies |
|
|
|
Allele 1 |
33 (34.7%) |
85 (89.5%) |
|
Allele 2 |
62 (65.3%) |
10 (10.5%) |
|
P. value |
0.011 |
|
|
Table 8: Genotype distribution of IL-1α (+4845), IL-1β (+3954), and TNF-α (-308) in AgP patients and healthy controls according to the gender. |
||||||
|
Genotypes |
Male |
T. value (95% CI) |
Female |
T. value (95% CI) |
||
|
IL 1α |
Case |
Control |
Case |
Control |
||
|
1,1 |
6 (33.3%) |
25 (60.9%) |
2.742 (0.16-1.04)* |
10 (13%) |
28 (51.9%) |
5.425 (0.40-0.87)* |
|
1,2 |
4 (22.2%) |
11 (26.8%) |
41 (53.2%) |
21 (38.9%) |
||
|
2,2 |
8 (44.5%) |
5 (12.2%) |
26 (34%) |
5 (9.2%) |
||
|
Total |
18 (100%) |
41 (100%) |
77(100%) |
54(100%) |
||
|
IL 1β |
|
|||||
|
1,1 |
10 (55.6%) |
19 (45.2%) |
-2.057 (-0.95-0.013) * |
37 (48%) |
27 (50%) |
-.757 (-0.39-0.17) |
|
1,2 |
8 (44.4%) |
6 (14.6%) |
27 (35%) |
11 (20.4%) |
||
|
2,2 |
0 |
16 (39.0%) |
13 (17%) |
16 (29.6%) |
||
|
Total |
18 (100%) |
41(100%) |
77(100%) |
54(100%) |
||
|
TNFα |
|
|
|
|
|
|
|
1,1 |
4 (22.2%) |
21 (51.2%) |
0.147 (-0.44-0.52) |
20 (26%) |
24 (44.4%) |
-1.396 (-0.45-0.08) |
|
1,2 |
12 (66.6%) |
5 (12.1%) |
50 (65%) |
5 (9.3%) |
||
|
2,2 |
2 (11.1%) |
15 (36.5%) |
7 (9%) |
25 (46.3%) |
||
|
Total |
18(100%) |
41(100%) |
77(100%) |
54(100%) |
||
*Statistically significant at p<0.001
|
Table 9: Correlation between pocket index, CAL, and cytokines genotypes among cases |
|||||
|
Parameters |
PD |
CAL |
IL 1α |
TNFα |
IL 1β |
|
PD
|
1 |
.140 |
-.036 |
-.006 |
.012 |
|
. |
.177 |
.727 |
.957 |
.907 |
|
|
CAL |
.140 |
1 |
-.055 |
-.079 |
.048 |
|
.177 |
. |
.598 |
.444 |
.646 |
|
|
IL 1α |
-.036 |
-.055 |
1 |
-.057 |
-.033 |
|
.727 |
.598 |
. |
.582 |
.751 |
|
|
TNFα |
-.006 |
-.079 |
-.057 |
1 |
-.036 |
|
.957 |
.444 |
.582 |
. |
.731 |
|
|
IL 1β |
.012 |
.048 |
-.033 |
-.036 |
1 |
|
.907 |
.646 |
.751 |
.731 |
. |
|
 |
|
(A) |
 |
|
(B) |
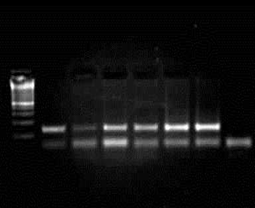
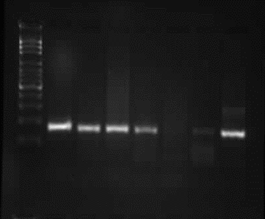
Figure 1: (A) the IL-1α+4845, and (B) the IL-1β+3954 PCR containing Single Nucleotide Polymorphisms (lanes 1-6) and their corresponding restriction endonuclease digestion fragments after agarose gel electrophoresis
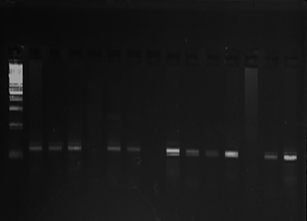
Figure 2: TNFα containing Single Nucleotide Polymorphisms (lanes 1-9) and its corresponding restriction endonuclease digestion fragments after agarose gel electrophoresis
DISCUSSION:
The current study is of significant value as it endeavors to study the genotype of IL-1α +4845, IL-1β +3954, and TNF-α-308 alleles among patients with aggressive periodontitis in Sudan. The patients’ population of this study was selected from those referred to Khartoum Dental Teaching Hospital during the period of the study. The prevalence of AGP was much higher (2%) than that of a previous epidemiological study of aggressive periodontitis in African populations. In Nigeria studies conducted in Lagos and Ibadan, the prevalence of aggressive periodontitis was 1%, 1.56%, respectively [19, 20]. In Sudan, Elamin AM et al. [21] reported that about 3.4% of the subjects selected from 38 public and private high schools of Khartoum had aggressive periodontitis. Abdalla Saleh et al. in 2017 noted that the prevalence of periodontitis in the Sudanese population was 1.4% [22]. The prevalence rate reported in the present study is also higher than that reported in a Koreans study on the prevalence of aggressive periodontitis (1.65%) [23]. Among Caucasians, the prevalence of aggressive periodontitis was 0.1% in northern and central Europe, 0.5% in southern Europe, and (0.1-0.2%) in North America [24]. The different result achieved in the present study compared to other studies regarding the prevalence of aggressive periodontitis worldwide may be due to the difference in criteria used (patterns and severity of attachment loss, microbial and immunological assay), clinical methods for measuring the periodontal attachment (visual assessment, radiographs, various periodontal indices, and probing), the types of the population studied (patients, school children, military, young adults), the age of the individuals assessed, and the sample selection method. Any combination of these differences could explain the variation in the prevalence rate, in addition to other factors including cultural and ethnic backgrounds.
A significant association was found between gender and aggressive periodontitis in this study. Female patients were found to be 4 times more likely to have aggressive periodontitis than male patients. Our findings support the evidence presented by Cho who reported a 1:2.5 male:Female ratio [23]. However few studies showed no difference in the prevalence of aggressive periodontitis between males and females [25]. The possible reason is that fluctuation in the amount of female sex hormones of estrogen and progesterone are responsible for different physiological changes in females at particular phases of their lives. These variations also influence other areas of the body, and therefore have a major effect on oral tissues, since estrogen and progesterone receptors have been found in the gingiva, periosteal fibers, and periodontal ligament fibroblasts and osteoblasts illustrating the direct action of female sex hormones on periodontal tissues [26].
The present study revealed that subjects from the Western Sudan States showed a higher number of aggressive periodontitis patients (38.9%), followed by Northern States (34.7%). However, Eastern States showed less percentage (3.2%). This supports the results reached by Ghandour, et al. (1999) who examined 5405 subjects for periodontal disease in Seven States of Sudan, and found that the distribution of periodontal disease in the different states comes in the same sequence [27]. These findings may be for the following reasons; Western states are rural and underdeveloped regions, with low hygiene behavior, unavailable medical services, as well as genetic predisposition. The prevalence of aggressive periodontitis varies significantly between populations, and differences in race/ethnicity seem to be a key factor. Many studies consistently show that aggressive periodontitis is most prevalent in Africa and in populations of African adolescents and is least prevalent in Caucasians in Europe and North America, as well as Arab populations [28]. Our study showed that the patients of Africans origin were twice likely to have aggressive periodontitis than Afro –Arab and other groups, which supports the global report that indicates the incidence of AgP differs throughout various races and racial groups that indicate genetic differences with ethnicity [29].
The findings of the current study revealed that there is a significant increase in the frequency of the IL-1α (+ 4845) genotypes consisting of allele 2 (IL-1α-889) with homozygous genotype 2,2 in aggressive periodontitis, as well as the predominance of heterogeneity as compared to the control group. However, homozygosity of 1,1 allele was more prevalent among the control group. This result more or less means that of the IL-1α (+4845) gene polymorphism especially (2,2) homozygous allele and heterozygous allele carriers have a crucial role in the pathogenesis, and progression of aggressive forms of periodontitis, since the study participants had observable signs of bacterial colonization (biofilm), as a result, the immune response was intensified as the entire blood is contaminated by periodontopathic bacteria or by-products. Our findings come in contact with one study reported that heterozygosity for allele 1 of IL-1α +4845 was related to increased susceptibility for AgP [30]. However, our result is in contrast with various studies that have been proceeded; evaluating the role of IL-1 gene polymorphism as a possible factor in periodontitis in various population and ethnic groups [12, 13].
On the other hand, we found no significant correlation between IL-1β (+3954) genotypes distribution and allele frequencies for study groups, as there was a convergence of results in the study populations whereas the IL-1β (+3954) percentage of homogeneous alleles 1,1 in patients was close to the those in the control group. A later investigation of African Americans with localized JP indicated that the prevalence of IL-1β + 3953 allele 1 in both cases and controls and was not significantly correlated with the disease [31]. In South America, IL-1 polymorphisms in AgP have been investigated among Brazilians and Chileans. IL-1 polymorphisms did not appear to play a role in periodontitis susceptibility in a Brazilian family with siblings diagnosed with AgP [32]. Another study reported that the T allele of IL-1β + 3954 was more prevalent in CP than AgP in a population group from the south-eastern region of Brazil [32]. The variations in the outcome of the different studies related to the risk of periodontal disease development are not the same for all populations. Clinical studies have already shown that the frequency of aggressive periodontitis differs significantly between races, regions, and countries [33]. A researcher [34] concluded that IL-1 genotype-positive individuals are 2.7 times more likely to have tooth loss than genotype-negative people, and has shown that differences in the progression of periodontitis in genotype-positive individuals may be due to several factors such as smoking. Hence, IL-1 positive genotypes play a significant role in the development of AgP compared with positive subjects, and microbial species became elevated when positive IL-1 genotypes were identified.
With regard to TNF-α SNPs at positions of -308, we found a significant correlation (p-value=0.001) of allele frequency among study participants, however, we failed to find a significant association between homozygous and heterozygous genotypes distribution in the study subjects. That is to say that individuals carrying allele 2 of TNF-α -308 may have more likely to develop aggressive periodontitis. This finding comes in contact with a global report done by Graves DT et al. [16] who concluded that the degradation of fibroblasts that appears during periodontal pathogen infection is partially controlled by TNF. As a result, much of the damage occurring during periodontal tissue degradation can be due to IL-1 and TNF production. This damage might indeed reflect an exaggerated response of the host response to periodontal pathogens triggered by the increased production of IL-1 and TNF. In addition, Majumder et al. [35] noted that TNF-a-308n2 is a potential risk linked to the incidence of both aggressive and chronic periodontitis. Put differently, Fassmann et al. and Scapoli et al. [36, 37] proved that TNF-a (308G / A) polymorphism did not correlate with chronic periodontitis patients. Finally, it has become obvious that there is a strong correlation between pre-inflammatory cytokines and aggressive periodontitis, and an individual's genetic profile plays a major role in initiating and progression course of the disease.
CONCLUSIONS:
The current study provides a significant clue that the IL-1α and IL-1β gene polymorphisms are correlating with AgP in the Sudanese population, the genotype of IL-1β remains a considerable risk factor for AgP. The study revealed a high prevalence rate of aggressive periodontitis (2%), and it is significantly age, gender, and ethnic associated disease.
Limitations of the study:
The present study considered only a total of 4687 (1563 male and 3125 female) participants, as the Sudanese population more than 30 million people according to the last Census. Many of the variables investigated depended on patients' reports such as oral hygiene habits, and medication used. This study did not incorporate the culture of bacteria, as well as investigation of the possible role of the level of anti-inflammatory cytokines in blood and gene polymorphism, Extensive clinical and epidemiological research efforts regarding more cytokines gene analysis are recommended.
ACKNOWLEDGMENT
This publication was supported by the Deanship of scientific research at Prince Sattam bin Abdul-Aziz University. Special thanks extended to Al Neelain University Faculty of Dentistry
Conflict of interest: The author declares that there is no competing interest.
Research funding: None declared.
Authors’ contribution:
- FA (sample collection, laboratory work, and purchasing reagents)
- WA (supervision)
- IG ( Supervision)
- SA(Laboratory works, and Calibration of machines, preparation Study protocol and SOPs)
- LE (Scientific writing of manuscript, and publication)
- YM (Statistical analysis of data)
- HAW (proofreading and review).
REFERENCES
- Nainggolan M, Sinaga NH, Suwarso E. The effect of Ethanol Extract Oak Gall (Quercus Infectoria G. Olivier) on the Cellular immune response of Mice. J. Adv. Pharm. Educ. Res. 2018;8(1):135-9.
- Mohy AA, Aljanaby AA, Al-Hadraawy SK. Serum concentrations of CD4+ and CD8+ in patients infected with scabies caused by Sarcoptes scabiei. J. Adv. Pharm. Educ. Res. 2018;8(1):121-6.
- Vigneshwar T, Ramesh S, Priya V. Inhibition of RagB gene using herbal compounds in the treatment of primary endodontic pathogenesis caused by Porphyromonas species-An in silico study. J. Adv. Pharm. Educ. Res. 2017;7(3):308-12.
- Haripriya S, Ajitha P. Antimicrobial efficacy of silver nanoparticles of Aloe vera. J. Adv. Pharm. Educ. Res. 2017;7(2):163-7.
- Brett PM, Zygogianni P, Griffiths GS, Tomaz M, Parkar M, D’Aiuto F, Tonetti M. Functional gene polymorphisms in aggressive and chronic periodontitis. J Dent Res. 2005;84(12):1149-1153. doi:10.1177/154405910508401211
- Childers NK, Grenett H, Morrow C, Kumar R, Jezewski PA. Potential Risk for Localized Aggressive Periodontitis in African American Preadolescent Children. Pediatr Dent. 2017;39(4):294-298.
- Chan-Myung Cho, Hyung-Keun You, Seong-NyumJeong. The clinical assessment of aggressive periodontitis patients.J Periodontal Implant Sci. 2011; 41(3): 143–148.
- Brigido JA, da Silveira VR, Rego RO, Nogueira NA. Serotypes of Aggregatibacteractinomycetemcomitans in relation to periodontal status and geographic origin of individuals – a review of the literature. Med Oral Patol Oral Cir Bucal. 2014; 19(2):e184.
- Faveri M, Figueiredo LC, Duarte PM, Mestnik MJ, Mayer MP, Feres M. Microbiological profile of untreated subjects with localized aggressive periodontitis. J Clin Periodontol. 2009;36(9):739-74 doi:10.1111/j.1600-051X.2009.01449.x
- da Silva MK, de Carvalho ACG, Alves EHP, da Silva FRP, Pessoa LDS, Vasconcelos DFP. Genetic Factors and the Risk of Periodontitis Development: Findings from a Systematic Review Composed of 13 Studies of Meta-Analysis with 71,531 Participants. Int J Dent. 2017;2017:1914073. doi:1155/2017/1914073
- Li Y, Xu L, Hasturk H, Kantarci A, DePalma SR, Van Dyke TE. Localized aggressive periodontitis is linked to human chromosome 1q25. Hum Genet. 2004;114:291–297. [PubMed] [Google Scholar]
- Papapanou PN, Neiderud AM, Sandros J, Dahlen G. Interleukin-1 gene polymorphism and periodontal status.A case-control study. J Clin Periodontol. 2001;28(5):389–96. [PubMed] [Google Scholar]
- McDevitt MJ, Wang HY, Knobelman C, Newman MG, Di Giovine FS, Timms J, Duff GW, Kornman KS. Interleukin-1 genetic association with periodontitis in clinical practice. J Periodontol. 2000;71(2):156–63. [PubMed] [Google Scholar]
- Greenstein G, Hart TC. A critical assessment of interleukin-1 (IL-1) genotyping when used in a genetic susceptibility test for severe chronic periodontitis. J Periodontol. 2002; 73(2):231-247. doi:10.1902/jop.2002.73.2.231
- Boch JA, Wara-aswapati N, Auron PE. Interleukin 1 signal transduction--current concepts and relevance to periodontitis. J Dent Res. 2001;80(2):400-407. doi:10.1177/00220345010800020101
- Graves DT, Cochran D. The contribution of interleukin-1 and tumor necrosis factor to periodontal tissue destruction. J Periodontol. 2003;74(3):391-401. doi:10.1902/jop.2003.74.3.391
- Taylor PC, Williams RO, Feldmann M. Tumour necrosis factor alpha as a therapeutic target for immune-mediated inflammatory diseases. Curr Opin Biotechnol. 2004;15(6):557-563. doi:10.1016/j.copbio.2004.09.005
- Wei XM, Chen YJ, Wu L, Cui LJ, Hu DW, Zeng XT. Tumor necrosis factor-α G-308A (rs1800629) polymorphism and aggressive periodontitis susceptibility: a meta-analysis of 16 case-control studies. Sci Rep. 2016;6:19099. Published 2016 Jan 11. 6(1):1-8. doi:10.1038/srep19099
- Akeredolu PA, Ayanbadejo PO, Nwhator SO, Savage KO. Prosthetic management of patients with juvenile periodontitis at the Lagos University Teaching Hospital. Nig Qt J Hosp Med. 2005;15(3):136–42. [Google Scholar]
- Arowojolu MO, Nwokorie CU. Juvenile periodontitis in Ibadan, Nigeria. East Afr Med J. 1997;74(6):372–5. [PubMed] [Google Scholar]
- Elamin A, Albander JM, Poulsen K, Ali RW, Bakken V. Pervalence of aa with Sudanese patients with aggressive periodontitis : a case –control study. Jou periodontal Res. 2011;46(3):285-91.
- Abdalla A S, Aloutabi A A. Tribal Distribution of Aggressive Periodontitis in Sudanese School Children (12-16 years) in Khartoum State. American Journal of Medicine and Medical Sciences. 2017; 7(9): 338-343.
- Cho CM, You HK, Jeong SN. The clinical assessment of aggressive periodontitis patients. J Periodontal Implant Sci. 2011;41(3):143-148. doi:10.5051/jpis.2011.41.3.143
- Joshipura, V.; Yadalam, U.; Brahmavar, B. Aggressive periodontitis: A review. Journal of the International Clinical Dental Research Organization. 2015; 7 (1).
- Goncalves PF, Harris TH, Elmariah T, Aukhil I, Wallace MR, Shaddox LM. Genetic polymorphisms and periodontal disease in populations of African descent: A review. Journal of periodontal research. 2018;53(2):164-73.
- Amar S, Chung KM. Influence of hormonal variation on the periodontium in women. Periodontol 2000. 1994;6(1):79-87. doi:10.1111/j.1600-0757.1994.tb00028.x.
- Ghandour IA, Ibrahim YE. A National Oral Health Plan for Sudan year 2001- 2005. Assignment report 1999. CSA 99/165.
- Susin C, Haas AN, Albandar JM. Epidemiology and demographics of aggressive periodontitis. Periodontol 2000 2014;65(1):27 45
- Praveena J, Battur H, Fareed N, Khanagar S, Bhat M. Inheritance patterns of localized aggressive periodontitis: A systematic review. J Indian Assoc Public Health Dent 2017;15(4):295-301.
- Guzeldemir E, Gunhan M, Ozcelik O, Tastan H. Interleukin-1 and tumor necrosis factor-alpha gene polymorphisms in Turkish patients with localized aggressive periodontitis. J Oral Sci. 2008;50(2):151–9. [PubMed] [Google Scholar]
- Walker SJ, Van Dyke TE, Rich S, Kornman KS, di Giovine FS, Hart TC. Genetic polymorphisms of the IL-1alpha and IL-1beta genes in African-American LJP patients and an African-American control population. J Periodontol. 2000;71(5):723–8. [PubMed] [Google Scholar]
- Trevilatto PC, Tramontina VA, Machado MA, Gonçalves RB, Sallum AW, Line SR. Clinical, genetic and microbiological findings in a Brazilian family with aggressive periodontitis. J Clin Periodontol. 2002;29(3):233–9. [PubMed] [Google Scholar]
- Moreira PR, de Sá AR, Xavier GM, Costa JE, Gomez RS, Gollob KJ, et al. A functional interleukin-1 beta gene polymorphism is associated with chronic periodontitis in a sample of Brazilian individuals. J Periodontal Res. 2005; 40(4):306–11. [PubMed] [Google Scholar]
- McGuire MK, Nunn ME. Prognosis versus actual outcome. IV. The effectiveness of clinical parameters and IL-1 genotype in accurately predicting prognoses and tooth survival. J Periodontol. 1999; 70(1):49–56. [PubMed] [Google Scholar]
- Majumder P, Thou K, Bhattacharya M, Nair V, Ghosh S, Dey SK. Association of tumor necrosis factor-α (TNF-α) gene promoter polymorphisms with aggressive and chronic periodontitis in the eastern Indian population. Biosci Rep. 2018; 38(4): BSR20171212. Published 2018 Jul 31. doi:10.1042/BSR20171212
- Fassmann A, Holla LI, Buckova D, Vasku A, Znojil V, Vanek J. Polymorphisms in the 1252 (A/G) lymphotoxin alpha and the 308 (A/G) tumor necrosis factor-alpha genes and susceptibility to chronic periodontitis in a Czech population. J Periodontal Res. 2003; 38(4):394_399.
- Scapoli C, Mamolini E, Trombelli L. Role of IL-6, TNF-A and LT-A variants in the modulation of the clinical expression of plaque-induced gingivitis. J Clin Periodontol. 2007; 34(12):1031-1038. doi:10.1111/j.1600-051X.2007.01145.x.
