Archive \ Volume.11 2020 Issue 2
Polycystic Ovarian Disease or Polycystic Ovarian Syndrome: How to Identify and Manage- A Review
Neha Minocha
School of Medical and Allied Sciences, K.R. Mangalam University, Sohna Road, Gurugram, Haryana, India.

Abstract
PCOD or PCOS is a reproductive and metabolic disorder concerned with the ovaries. An ovary is an active organ that changes its form, appearance, and shape according to its hormonal ambiance. PCOD or PCOS is a condition in which ovary of women of childbearing age is enlarged and starts producing an excessive amount of male hormones (androgens) and is the main cause of infertility, diabetes, irregular menstrual periods, and hirsutism. No exact cause of the disease has been found yet but the change in lifestyle, change in dietary needs, lack of exercise, and the most important of all, i.e. stress level induces the disease. There are medicines, which can induce an artificial menstrual cycle and regulate the level of hormones and ultimately treat the three signs of PCOS i.e. Acne, Hirsutism, and Obesity.
Keywords: PCOD, PCOS, ovulatory dysfunction, hyperandrogenaemia, hirsutism

INTRODUCTION
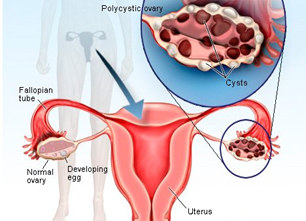
PCO (Polycystic ovary) is a condition and PCOS (Polycystic ovary syndrome) is a symptom [1, 2]. A pattern of symptoms belonging to a particular disease is defined as a syndrome [3]. Ovary of normal women who is in the age of her reproductive years has a volume of around 4-6 ml of each ovary and have a folded structure like a walnut, but if a woman is diagnosed with PCOS, her ovaries get enlarged and bulky with having more than 10 ml of volume, thus it starts producing a high quantity of androgens [4-10].
Normal ovulating ovaries contain fluid-filled sacs called follicles, with variations in size from 1 to 30 millimeters, which depends on the phase of the menstrual cycle. The individual sac or follicle contains a tiny egg, which never matures enough to trigger ovulation. While in the polycystic ovary, there are more than 12 small follicles, measuring 2 to 9 millimeters in diameter, and are usually arranged in a ‘pearl-necklace’ manner around the periphery [11]. So, as the name suggests, poly means many, in polycystic ovary syndrome there are many small cysts like sacs that are filled with fluids and grown inside the ovaries and they do not need to be removed surgically.
 |
 |
|
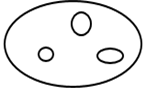
Normal Ovary |
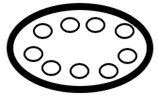
Polycystic Ovary |
|
Fig 1: Normal & polycystic ovary |
|
|
Fig 2: Inside view of Polycystic ovaries |
|
Features
The vital features of PCOS are excessive production of male hormones and having many cysts in the ovaries. However, a few common problems that women diagnosed with PCOS may include the following:
- Hirsutism: the presence of excess hair on the body
- irregular or missing periods
- heavy periods
- acne, oily skin, and other skin related problems
- hair loss and hair thinning from the scalp
- insulin resistance
- fertility problems
- body weight-related issues [3].
But these features do not rely on if a patient may have polycystic ovaries or may have PCOS. In 2003, a meeting was held by experts and they revised their concern about the PCOS, which later on they get their work published in 2004, which concluded: ‘PCOS is a syndrome of ovarian dysfunction and its basic features include hyperandrogenism and polycystic morphology’ [6].
History
Polycystic ovaries were described as early as the 19th century but it was not until 1935 that syndrome was identified and subsequently named for Stein and Leventhal, who first associated with amenorrhea, obesity, and hirsutism with polycystic ovaries in seven patients and thus PCOS syndrome was initially termed as Stein–Leventhal syndrome [12, 13].
Before their research, dating back in 1721, young married women, infertile and moderately obese had their ovaries of larger size and bulky than normal were identified but then also it was not recognized. In 1844, Chereau described the sclerocystic changes in ovaries yet it was not recognized until Stein and Leventhal had comprehensive research on it [13].
In 1985, another research was carried out by Adams and his colleagues and they noticed polycystic ovaries with an excessive number of follicles and termed that condition multifollicularity. According to them, polycystic ovaries are those in which there is the presence of more than 10 cysts having 2–8 mm diameter and are peripherally arranged [13].
ETIOLOGY: The exact etiology of PCOS or PCOD is yet to be explicated; nevertheless there is noticeable inherent resistance towards insulin, even if the women are slender [14, 15]. Following hyperinsulinemia (increase in insulin level), which increases the production of androgen; there is a decrease in protein binding, which ultimately increases the level of free androgen. Due to the above-mentioned hormonal imbalance, there are noticeable alterations in the appearance of the ovary, disturbing its function and hurts fertility [16-19].
Insulin resistance concerning PCOS is further worsened by obesity [20]. Obesity is having a two-directional relationship with PCOS, with women gaining weight regularly, exacerbates PCOS occurrence and its severity. PCOS reacts well to exercise and having a change in the dietary plan, both of which reduce insulin resistance [16].
Some features highlighted by findings that androgen secretion is stimulated by insulin via ovarian theca, which suppresses (SHBG) sex hormone-binding globulin and, thus, enhances free circulating testosterone [12]. However, insulin resistance is not considered a universal feature of PCOS [21].
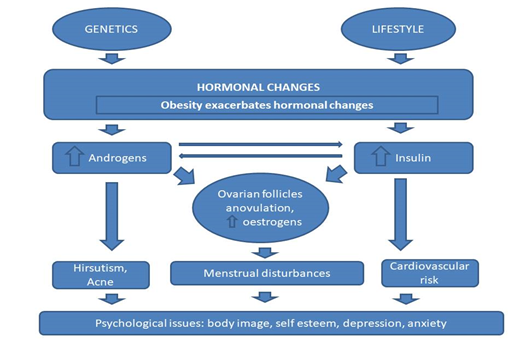
Fig 3: The etiological, hormonal and clinical features of PCOS
Pathophysiology
As mentioned above, the fundamental pathophysiological defect concerning PCOS is not known, but some of the important features include resistance to insulin, excess production of androgen, and transformed gonadotropin dynamics [22]. Organs that are affected by PCOS are a woman’s ovaries, it is the reproductive organ through which estrogen and progesterone hormones are produced and ultimately menstrual cycle is regulated. It is a myth that women do not need for male hormones but the fact is ovaries produce a negotiable amount of male hormones that we call as androgens. In PCOD, there are elevated levels of Luteinizing Hormone, which is three times higher than Follicle Stimulating Hormone, which ultimately leads to increased production of testosterone by the ovaries leading to the growth of facial hair and acne [23].
It is also associated with an imbalance in glucose and insulin dysfunction, which leads to obesity, diabetes, a rise in cholesterol level, and an increase in blood pressure. Thus increased production of androgen blocks the ovulation process and causes follicular atresia (Growth of follicles is arrested), before the pre-ovulatory phase. Also, if women take a diet, which is high in carbohydrate and fat content then weight gain resulting from dietary plan seems to exacerbate the signs of PCOS. Women having PCOD are at high risk of developing diabetes, cardiovascular diseases, infertility, and endometrial cancer [24, 25].
Cause
No exact cause of PCOD or PCOS has been found yet, but yes there are certain points, which correlate the cause of PCOD and these are the patient’s family history (genetic), her change in lifestyle, lack of daily routine exercise, changes in dietary habits, loss of work-life balance, exposure to environmental pollution, exposure to mobile phone radiations, and the most important of all is stress [26]. Stress levels in humans are increasing day by day and, thus, it has now developed as one of the primary causes of PCOD, which can ultimately lead to a rise in blood pressure (hypertension), diabetes mellitus (most commonly Type-2 diabetes), increased risk of uterine cancer and many cardiovascular diseases [22, 24, 25, 27]. Researchers are still trying to discover if any gene is responsible or might be linked to PCOS or PCOD. Some women, who are obese, having severe excess body hair and raised blood levels, yet have a perfectly regular menstrual period [26]. And many women are thin but have PCOS, which reminds that the exact cause or the exact story about PCOS is not confirmed. When women eat lots of carbohydrates the level of insulin in the body is increased, which increases the level of testosterone and decreases SHBG (a protein to which testosterone attaches) level in ovaries and liver respectively. Changes in testosterone and SHBG levels elevate free testosterone levels, which ultimately leads to irregular periods and skin problems [28, 29].
Certain causes of disordered ovulation, hirsutism, and acne are listed below:
- Genetic
- Nutritional
- Intrauterine
- Hormonal
- Fat, insulin, skin sensitivity [26].
Diagnosis:
Since PCOS is a syndrome and cannot be diagnosed by single diagnostic criteria, it is identified by any two out of the following three clinical criteria, because women having PCOD may have:
- Oligomenorrhoea (irregular or prolonged menstrual cycles)
- Hyperandrogenism (excessive production of androgens)
- The polycystic appearance of the ovaries (multiple follicles in the ovary)
Oligomenorrhoea is a condition when there is a skip of more than 3 menstrual cycles or we can say that irregular menstrual cycle. There are several blood tests, which are done to check the menstrual irregularities and these are levels of Luteinising Hormone (LH), Follicle Stimulating Hormone (FSH), TSH, and Prolactin, which is known as PCOD panel as all these laboratory tests are done under PCOD Panel. Hyperandrogenism is when there is excess production of androgens, which is exposed by acne, oily skin, and excess hair on the face, chest, and stomach [6, 16, 30]. While in some cases, women face hair thinning and baldness, but it could be a sign of underactive thyroid, malnutrition, iron or zinc deficiency, stress, sickness or a problem of PCOS also. Polycystic ovaries mean when there are several present small sized follicles around the periphery or near the ovarian surface which is diagnosed by ultrasonography [11, 31]. If there is a reverse ratio of FSH: LH (3:1), then it may be PCOD. Endocrine features related to the diagnosis of PCOS include an elevated level of certain hormones like androgens, luteinizing hormone, prolactin, and estrogen [32]. A lowering of vitamin D level also exacerbates PCOD [16].
A doctor must be able to see the ovaries while investigating for polycystic ovaries and this can be done by using abdominal ultrasound, vaginal ultrasound and/or laparoscopy. In abdominal ultrasound, a map of the area being scanned by using soundwaves and investigate the ovaries. Though this method is painless ovaries are not visible so vaginal ultrasound or laparoscopy is done to have a clear look at the ovaries. Vaginal ultrasound is not done in unmarried women, because it can be done using a vaginal probe, which is gently inserted into the vagina and placed right next to the wall of the ovary to get a clear look at the prominence of cysts. While laparoscopy, a cut in the naval is made and an extremely small telescope is allowed to enter through the cut and allow the surgeon to have a clear and complete look at ovaries, uterus, and fallopian tubes, and so on. With the help of laparoscopy, the doctor can get a good-quality picture of the desired part [33].
Treatment
There are many views regarding the treatment of PCOS, some say it cannot be treated as it is a life-long disorder and some concluded that having a change in lifestyle and having hormonal treatment can work well with PCOS [28]. Consequences related to health concerning PCOS are diverse and may include non-functioning or dysfunction of certain organs, so it is the utmost thing to get treated off this disorder and have a stress-free life. If a woman is obese, she may have a deficiency of vitamin-D, because obesity is directly linked with a decrease in the level of vitamin-D and that person may likely get osteoporosis or rickettsia [16]. Thus, the very first step in the treatment changes in lifestyle. There are certain lifestyle management strategies, which work well in PCOS:
- Prevent getting obese or being over-weight (having weight management)
- Modification in dietary routine by having a low-carbohydrate diet
- Regular physical activity or regular exercise
- Modification in behavior
- Stress -free lifestyle
- Reduce the intake of fast food
- Reduce intake of processed food
- Reduce the intake of alcoholic beverages
- Regular check on vitamin-D level [16, 26, 34]
Recent medicines used in regulating PCOS:
Certain medicines are used globally to regulate PCOS and the first line of pills that are used to prevent hirsutism, acne, and irregular menstrual periods are oral contraceptives. Oral contraceptives are the pills, which are appropriately composed of hormones and they start an artificial menstrual cycle in women so as she can get a withdrawal bleeding. Contraceptive Pills come in a pack of 21 active tablets, and some then have seven days of inactive tablets as a reminder to have a seven-day break from the medication. These pills also possess good treatment for excess hair and acne because they contain a small dose of male hormone blockers. These pills result in very low levels of free testosterone in the body. While having these pills, one cannot get pregnant. In the market, there are many brands of the pills available and these are:
- Diane-35 (contain a small amount of synthetic progestin, CPA)
- Yasmin (contain a small amount of synthetic progestin)
- Marvelon
- Femoden-ED
- Microgynon
Some drugs that contain CPA Cyproterone acetate, are enormously useful drugs for the management of severe androgen-excess disorders. CPA is an androgen-blocker—which means it suppresses the ovarian production of testosterone—and it is a progestin, so it protects the uterus against cancer and lightens menstrual periods. It is usually given with estrogens [35].
Recent advances in the management of pcos
PCOS appears to be a heterogeneous condition and whose initial management of diagnosis of PCOS or PCOD will depend on the clinical problems (anovulation or hirsutism).
- Hirsutism: The backbone of managing PCOS largely depends on hair removal techniques. In some cases, this may still be the choice of treatment if fertility is sought. In the 1960s, antiandrogen therapy was introduced in which spironolactone, cyproterone acetate, and more recently flutamide are successfully used in treating symptoms of hyperandrogenism, which also includes acne. To induce regular withdrawal of bleeding in patients having PCOS, antiandrogens are usually prescribed with a low-dose oral contraceptive.
- Anovulation: In 1958, the first human pituitary FSH was used to induce ovulation in anovulatory women but it was stopped afterward because it was causing severe complication rates to both fetus and mother. Afterward, in 1961, Greenblatt and his associates stated positive induction of ovulation using clomiphene citrate, which is chemically related to the non-steroidal estrogen chlorotrianisene. Clomiphene citrate was used because it was inexpensive and had low toxicity with fewer side effects. Likewise, after several approaches like the introduction of GnRH analogs were developed but all of them possess serious problems.
The next medical treatment was ovulation induction with metformin, an insulin-sensitizing agent, which decreases the insulin level and lowers the level of circulating total and free androgen with a result in improving clinical sequelae of hyperandrogenism.
- Weight loss: In modern society, changes in the dietary routine can increase the proportion of obesity among women and also the symptoms of PCOS as an excess of body fat emphasize insulin resistance. Obese women with PCOD have irregular ovulation and hyperandrogenism and thus making treatment less effective and less efficient. Weight loss will lead to certain improvements in management [36].
Remedies
- Lifestyle modification
- Dietary changes
- Insulin-lowering drugs
- Oral contraceptives
- Weight loss
- Progestin therapy
- Medicines for hirsutism
- Fertility medications.
CONCLUSION
PCOD or PCOS is a reproductive disorder in which women’s ovary gets enlarged and starts producing an excessive amount of male hormones (androgens) and is the main cause of infertility, diabetes, irregulation in menstrual periods, and hirsutism. The pathophysiologic defect is not known yet, but certain vital features are known, which include resistance towards insulin, an increase in the level of androgen production, and altered gonadotropin dynamics. It is also associated with an imbalance in glucose and insulin dysfunction, which leads to obesity, diabetes, a rise in cholesterol level and an increase in blood pressure. Stress is one of the primary causes of PCOS, which can ultimately lead to hypertension, diabetes mellitus, increased risk of uterine cancer, and even cardiovascular diseases. Endocrine features related to the diagnosis of PCOS or PCOD include elevated levels of certain hormones like androgens, luteinizing hormone, prolactin, and estrogen. Diagnostic criteria of the disease are having two out of the following symptoms: Hyperandrogenism, Oligomenorrhoea, or Polycystic appearance of the ovaries. Infertility, menstrual disturbances, and acne can be prevented by taking oral contraceptives, insulin lowering drugs, progestin therapy, and weight loss.
REFERENCES
- Polycystic Ovary Syndrome: A woman’s guide to identifying and managing PCOS, Dr. John Eden; 2005:
- Osman NN, Alsahfi SA, Alshubaily F. Effectiveness of Aqueous Extract of Fenugreek Seeds and Flaxseed on Polycystic Ovarian Syndrome in Female Rats. Int. J. Pharm. Res. Allied Sci. 2019;8(4):42-54.
- Polycystic Ovary Syndrome: A woman’s guide to identifying and managing PCOS, Dr. John Eden; 2005:4.
- Adams J, Polson DW, Franks S. Prevalence of polycystic ovaries in women with anovulation and idiopathic hirsutism. Br Med J (Clin Res Ed) 1986;293:355-9
- Balen A. Pathogenesis of polycystic ovary syndrome–the enigma unravels? Lancet 1999;354:966-7
- Michelmore KF, Balen AH, Dunger DB, Vessey MP. Polycystic ovaries and associated clinical and biochemical features in young women. Clin Endocrinol (Oxf) 1999;51:779-86
- Legro RS. Polycystic ovary syndrome: current and future treatment paradigms. Am J Obstet Gynecol 1998;179(Suppl):101-8
- Tsilchorozidou T, Overton C, Conway GS. The pathophysiology of polycystic ovary syndrome. Clin Endocrinol (Oxf) 2004;60:1-17
- Balen AH. Is metformin the treatment of choice for anovulation in polycystic ovary syndrome? Nat Clin Pract Endocrinol Metab 2007;3:440-1
- Poordast T, Alborzi T, Askari E, Samsami A, Najib FS, Hamedi M, Naghmeh Sanj Z. A Rare Case of Tubo-Ovarian Abscess by Enterococcus SPP, Following Intrauterine Insemination. Int. J. Pharm. Phytopharm. Res. 2019;9(2):32-5.
- Polycystic Ovary Syndrome: A woman’s guide to identifying and managing PCOS, Dr. John Eden; 2005:3.
- PonJola Coney, Polycystic ovarian disease: current concepts of pathophysiology and therapy, Fertility And Sterility;1984 (42): 667-680
- Polycystic Ovary syndrome, Gabor T. Kovacs and Robert Norman, Cindy Farquhar; 2007:4-7.
- Stepto NK et al. Women with polycystic ovary syndrome have intrinsic insulin resistance on euglycaemichyperinsulaemic clamp. Hum Reprod. 2013;28(3):777–784.
- Dunaif A. Insulin resistance and the polycystic ovary syndrome: Mechanism and implications for pathogenesis. Endocr Rev. 1997;18(6):774–800.
- Thomson RL, Teede HJ, Stepto NK, Banting LK, Moran LJ. 2 The Role of Diet and Lifestyle Modification in the Treatment of Polycystic Ovary Syndrome. InNutrition, Fertility, and Human Reproductive Function 2015 Feb 24 (pp. 42-65). CRC Press.
- Goodarzi MO et al. Polycystic ovary syndrome: Etiology, pathogenesis, and diagnosis. Nat Rev Endocrinol. 2011;7(4):219–231.
- Teede HJ et al. Assessment and management of polycystic ovary syndrome: Summary of an evidence-based guideline. Med J Aust. 2011;195(6): S65–S112.
- Teede H, Hutchison SK, Zoungas S. The management of insulin resistance in polycystic ovary syndrome. Trends Endocrinol Metab. 2007;18(7):273–279.
- Jassim WH, Al-Obaidi MT, Abdulhameed WA. The Effect of Insulin Resistance on Oocyte Maturation and Embryo Quality in PCOS Patients Undergoing ICSI. Int. J. Pharm. Phytopharm. Res. 2019;9(1):36-42.
- Polycystic Ovary Syndrome: A woman’s guide to identifying and managing PCOS, Dr. John Eden; 2005:172.
- Guzick David, Polycystic ovary syndrome: Symptomatology, pathophysiology, and epidemiology;1998:S89-S93.
- Polycystic Ovary Syndrome: A woman’s guide to identifying and managing PCOS, Dr. John Eden; 2005:48-49.
- Moran LJ et al. Impaired glucose tolerance, type 2 diabetes and metabolic syndrome in polycystic ovary syndrome: A systematic review and meta-analysis. Hum Reprod Update. 2010;16(4):347–363.
- Wild RA et al. Assessment of cardiovascular risk and prevention of cardiovascular disease in women with the polycystic ovary syndrome: A consensus statement by the Androgen Excess and Polycystic Ovary Syndrome (AE-PCOS) Society. J Clin Endocrinol Metab. 2010;95(5):2038–2049.
- Polycystic Ovary Syndrome: A woman’s guide to identifying and managing PCOS, Dr. John Eden; 2005:43-45.
- DuRant Elizabeth, Polycystic Ovary Syndrome: A Review of Current Knowledge; The Journal for Nurse Practitioners;2007:180-185.
- Polycystic Ovary Syndrome: A woman’s guide to identifying and managing PCOS, Dr. John Eden; 2005:183-185.
- Ashtiani AR, Vahidian-Rezazadeh M, Jafari M, Galdavi R, Mohammad M. Study of Changes in The Plasma Levels of Chemerin of Women with Overweight and Obese During a Period of Endurance Training On a Cycle-Ergometer Using Hydroalcoholic Extract of Urtica. Pharmacophores. 2018;9(2):72-9.
- Azziz Ricardo, Reproductive BioMedicine Online; PCOS: a diagnostic challenge;2004 (8):644-648.
- Alnahdi HS. The Possible Ameliorative Mechanisms of Curcumin and/or Coenzyme Q10 Against Hyperthyroidism Induced Liver Damage in Rats. Entomol. appl. sci. lett. 2018;5(1):7-16.
- Polycystic Ovary Syndrome: A woman’s guide to identifying and managing PCOS, Dr. John Eden; 2005:55-56.
- Polycystic Ovary Syndrome: A woman’s guide to identifying and managing PCOS, Dr. John Eden; 2005:19-24.
- Polycystic Ovary Syndrome: A woman’s guide to identifying and managing PCOS, Dr. John Eden; 2005:73-75.
- Polycystic Ovary Syndrome: A woman’s guide to identifying and managing PCOS, Dr. John Eden; 2005:103-115.
- Cindy Farquhar, Introduction and history of polycystic ovary syndrome; 2007:4-13.